Tuberculosis: Different types of immunity determine the course of the disease
Patients in the tuberculosis outpatient clinic at Katutura State Hospital in Windhoek, Namibia.
An international research team has succeeded in characterising different immune responses of tuberculosis patients and identifying groups of patients who either showed a very low or a very strong immune response to the bacterial pathogen. This classification could significantly improve personalised treatment options in the future. Scientists from the German Center for Infection Research (DZIF) played a key role in the large-scale analysis.
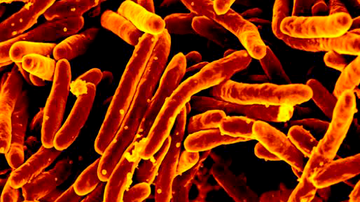
Tuberculosis is an infectious disease caused by Mycobacterium tuberculosis. The World Health Organization (WHO) estimates that a quarter of the world’s population is infected with this pathogen. Every year, more than 1.5 million people die from it. Tuberculosis is thus the most frequent cause of death caused by bacteria worldwide and is the second-highest cause of death from infectious diseases overall after COVID-19.
Interestingly, however, most people do not become ill after infection with Mycobacterium tuberculosis. For people who contract tuberculosis, the course of the disease can vary quite a bit. Most tuberculosis patients develop chronic pneumonia, but it may also affect lymph nodes, bones or the central nervous system in other patients. For decades, researchers have been studying the human response to tuberculosis bacteria in order to better understand what it takes to build protective immunity against this disease.
Now, researchers at Baylor College of Medicine and Texas Children’s Hospital in Houston, Texas (USA), in collaboration with partners at the German Center for Infection Research (DZIF), have made a ground-breaking discovery about human immunity to tuberculosis: using blood analyses, they were able to identify ‘endotypes’ among affected patients whose immunity was either too low or too pronounced.
For many years, doctors caring for tuberculosis patients have observed that some tuberculosis patients respond with a very strong immune system reaction, causing irreversible tissue and organ damage through excessive inflammation; conversely, the immune response in other patients appears to be too low to overcome the infection and kill the bacteria.
The model for the current analysis was derived from modern cancer research concepts. Large data sets from previously published papers were used to characterise the patients’ immune responses. The scientists focused on the different production of ribonucleic acids (RNA) in blood cells. With this information, they were able to identify certain groups among the tuberculosis patients who were associated with too low or too pronounced immunity. An interesting side note is that tuberculosis patients often suffer from an exhaustion of the immune system. The different groups are now categorised as ‘endotypes’.
In an independent cohort of patients from the DZIF tuberculosis cohort, the authors were able to demonstrate that one endotype had a better prognosis for curing tuberculosis than the other. Using computer models, the team also predicted what kind of drugs would be needed to rebalance the immune systems of the various endotypes. These types of personalised treatment concepts could lead to an enormous improvement in treatment results in the future and even shorten the treatment duration.
‘The host-specific immunotherapies we have identified will be beneficial for one of the endotypes, while they may be detrimental for patients with another endotype’, explains Professor Andrew DiNardo from the Baylor College of Medicine, who was the lead developer of the endotype concept. ‘The results of this study will pave the way for host-specific therapies for individual groups of tuberculosis patients, with great potential to improve treatment outcomes for the deadliest of all bacterial infectious diseases’, adds Professor Jan Heyckendorf, a DZIF tuberculosis researcher from Borstel and Kiel and one of the study’s lead authors.