Undetected and difficult to treat: multidrug resistant tuberculosis strain
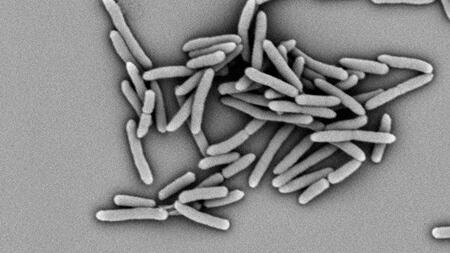
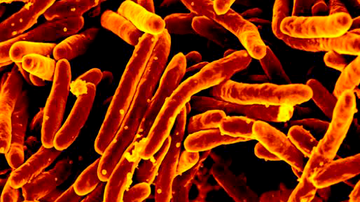
Scanning electron microscope image of a Mycobacterium tuberculosis strain at 13,000x magnification.
Scientists at the Research Center Borstel and the German Center for Infection Research (DZIF) identified a multidrug resistant Tuberculosis-strain in Southern Africa, that is not detected by modern diagnostic methods and has developed resistance to the new antibiotic bedaquiline and a repurposed drug, clofazimine. The results of this work have now been published in the journal Genome Medicine.
About 1.4 million people die worldwide every year as a result of tuberculosis (TB). One of the biggest problems in treatment is the increasing development of resistance: The triggering pathogen, Mycobacterium tuberculosis, is becoming increasingly insensitive to the antibiotics used - the bacteria can no longer be controlled with these drugs.
Eswatini (previously: Swaziland) in Southern Africa is also a country with a high TB rate (363 new cases per 100,000 inhabitants), with around nine percent of those affected being infected with a multiresistant variant. In this study that has been conducted under the leadership of scientists at the Research Center Borstel and the German Center for Infection Research with collaboration from different institutions, a total of 144 MDR-TB isolates collected in Eswatini over two periods (2009-2010, 2014-2017) were analyzed using whole genome sequencing. This analysis showed that more than 30% of the MDR TB isolates belong to one outbreak strain, which has a specific rifampicin resistance mutation not detected by the Xpert MTB/RIF rapid test and other molecular methods for resistance detection. Recent data from an independent study show that the outbreak strain with this specific mutation now accounts for more than 50% of MDR-TB isolates in Eswatini.
"The high proportion of this outbreak strain in the country is a major problem for the control of the MDR-TB epidemic in Eswatini", says senior author Prof. Stefan Niemann, Research Center Borstel and DZIF. "There is a considerable risk for the outbreak strain to spread further and seriously complicate treatment of the afflicted patients will due to its inherent resistance to most drugs used in tuberculosis therapy”.
The results challenge the role of molecular rapid tests such as Xpert MTB/RIF in regions with frequent occurrence of such isolates and underline the importance of methods that can detect all multiresistant TB cases, such as genome sequencing.
Source