How Epstein-Barr virus silences immune alarms signals of the host cell
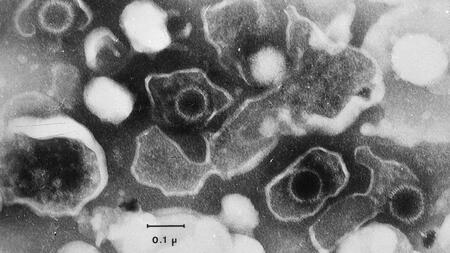
The Epstein-Barr virus (EBV)
Epstein-Barr virus (EBV) prevents infected cells from being attacked by the immune system. The virus drives production of small molecules, so-called microRNAs, that suppress alarm signals sent out by the infected cell. DZIF scientists at Helmholtz Zentrum München have elucidated this previously unknown mechanism.
The Epstein-Barr virus, first described by the English virologists Michael Epstein and Yvonne M. Barr, is found in the majority of the world’s population, but is usually held in check by the immune system. Nevertheless, the body is unable to eliminate this pathogen completely. The team of scientists led by Prof. Wolfgang Hammerschmidt, head of the Research Unit Gene Vectors at Helmholtz Zentrum München and a member of the German Center for Infection Research (DZIF), is striving to find out the reasons behind this.
Hide-and-seek: EBV makes itself invisible
“Our new studies show that by means of microRNAs, the virus prevents the infected cell from alerting the immune system,” said Hammerschmidt, summarizing the findings. MicroRNAs (miRNAs) are very short, noncoding RNAs that play an important role in gene regulation and especially in the silencing of genes. EBV usually hides in B cells, a class of white blood cells. If they are infected by EBV, the virus induces the cells to proliferate and thus to expand the reservoir of viruses. The B cells usually respond with an alarm signal to the immune system: They present molecules of the virus on their surface and secrete inflammatory cytokines to attract immune cells.
“It's just this alarm signal that's suppressed by microRNAs made by the virus,” said Manuel Albanese, a scientist in the Research Unit Gene Vectors. His colleague Takanobu Tagawa added: “The microRNAs block production of the proteins that would ring this alarm.” The two doctoral students share the lead authorship of the two publications in the Proceedings of the National Academy of Sciences and in the Journal of Experimental Medicine.
New approach may be promising for cancer therapy
Since the EBV virus drives division of B cells and thereby causes particular forms of cancer, the researchers are considering how to apply these findings to cancer therapy. “The mechanism we discovered renders killer T cells and helper T cells inactive, even when they directly face the infected cell,” said study leader Hammerschmidt. Killer T cells can destroy the infected cells, thus preventing the virus from multiplying. Helper T cells (also called CD4 T-cells) support them and also ensure the production of antibodies against the virus. “If it were possible to disrupt this blockade by EBV, this could be an interesting approach to treat cancer: the immune system could then better fight tumors that are triggered by EBV.“ For other diseases, clinical studies on active substances that shut off specific microRNAs have already started, the authors say.